NACC EXECUTIVE TEAM

NACC
EXECUTIVE TEAM
The Executive team of the NACC is composed of the Chairs of the respective NACC Subcommittees.
NACC & ITS MEMBERS

Yolanda
Simon

Ms. Heather
Rodney

Ms Jacqueline
Reid

Mr. Steve
Baras

Ms. Cyrus
Williams

Mr. Eswick
Padmore

Ms. Delores
Robinson

Ms. Dianna
Weekes

Ms. Kimberly
Gilbert
How It Began

OUR
HISTORY
The principles that guide the Trinidad and Tobago National HIV and AIDS Policy are aligned with those upon which Vision 2030 and the NSP are premised.
HIV and COVID-19
HIV &
COVID-19
COVID-19 is an infectious disease caused by the SARS-CoV-2 virus. This virus was discovered in China in 2019 and has continued to spread around the world, resulting in a global pandemic. There is currently no cure for COVID-19.
COVID-19 is transmitted when people breathe in droplets that have been exhaled by an infected person. In some cases, people may contract COVID-19 if they come into contact with contaminated body fluids that reach the eyes, nose or mouth.
Symptoms can range from mild to severe. In severe cases it causes respiratory symptoms, including difficulty breathing. COVID-19 can also affect other parts of the body, including causing body aches and joint pain, or causing gastrointestinal symptoms such as diarrhea and nausea.
In 2021, vaccines became available that prevent severe disease outcomes. In some countries, antiviral treatment can also help lessen the severity of the disease.
THE FACTS ABOUT COVID-19, HIV & YOU
COVID-19 And PLHIV
We are still learning about COVID-19 and how it affects people living with HIV, but we know that it is important for PLHIV to continue taking antiretroviral medications to keep the immune system healthy.
Talk with your care team to be sure you have an adequate supply of ART on hand.
For PLHIV who are virally suppressed, it is thought that COVID-19 affects this group about the same as the general population – that is, virally suppressed PLHIV are likely not at greater risk of contracting or experiencing severe COVID-19 illness.
For PLHIV who are unsuppressed, it is important to work with your care team to achieve viral suppression through good adherence and proper medications.
COVID-19 Signs and Symptoms
COVID-19 has several symptoms and signs. Many of these are very common and are associated with other illnesses.
Common symptoms include fever, tiredness, and a dry cough. Some people may also experience shortness of breath, a temporary loss of smell or loss of taste, or diarrhea. These symptoms usually resolve in approximately 10 days.
In severe cases persons may experience high fevers, pneumonia, and difficulty breathing.
It takes anytime between 1 and 12 days for symptoms to appear after exposure to the virus.
Many persons may never present with any of these signs or symptoms, known as asymptomatic cases.
COVID-19 Testing
If you are experiencing symptoms of COVID-19 (coughing, fever, shortness of breath, diarrhoea, loss of taste or smell), it is a good idea to get a COVID-19 test. For up-to-date information on where to access testing, review the Ministry of Health page on COVID-19 testing and screening.
COVID-19 Prevention
Practice basic COVID precautions:
Notify your health provider if experiencing symptoms. Follow their guidance about seeking care and quarantining.
For more information, visit the Ministry of Health COVID-19 information page on COVID-19 prevention.

COVID-19 Vaccination
You may be concerned about COVID-19, vaccinations, and HIV. In general, PLHIV who are virally suppressed typically respond well to vaccines.
COVID-19 vaccines bring the same benefits to PLHIV as they bring to all individuals and communities, including prevention of severe disease and the potential for reduced transmission of COVID-19.
The Ministry of Health offers additional information about COVID-19 vaccination, including information on where and how to get vaccinated.
If you have any other questions or concerns, reach out to your medical provider.
PREVIOUS TOPIC:
U and Your Baby HIV and Pregnancy
NEXT TOPIC:
Overview - U and Your Dream Team"
U and Your Baby - HIV and Pregnancy

U & YOUR BABY
HIV & PREGNANCY
Just as you can have a full life as a PLHIV, you can also give life. In this section, we examine all you need to know about HIV and pregnancy.
You may be wondering if you can have HIV and still have a baby. You most certainly can! You can enjoy the full benefits of parenthood as PLHIV. Let’s consider some questions that you may have.
THE FACTS ABOUT HIV, PREGNANCY & YOUR BABY
Can You Breastfeed If You Have HIV?
The current recommendation is that people living with HIV should NOT breastfeed or pre-chew food for their babies. Keeping an undetectable viral load greatly lowers, but does not remove, the risk of transmitting HIV through breastfeeding. If you have questions about breastfeeding or desire to breastfeed, talk to your doctor about infant feeding options. Mothers can certainly still preserve healthy bonds with their babies using other feeding methods.
What Is The Safest Way To Conceive?
Yes. A person living with HIV can transmit HIV to their baby any time during pregnancy, childbirth, or breastfeeding. Remember though that this doesn’t mean that you can’t have children. You just have to work closely with your Dream Team.
Following the guidelines regarding ART can prevent transmission of HIV to your baby and protect your health.
Are HIV Medicines Safe For You To Use During Pregnancy?
Yes - most HIV medicines are safe to use during pregnancy. While your pregnancy journey may feel private, talk with your doctor at your Treatment Site about the benefits and risks of specific HIV medicines during pregnancy or while you are trying to get pregnant.
Your Dream Team will be able to guide you well.
What Should You Ask Your Treatment Team About Having A Baby
You might ask your health care provider some of these questions:
What Are Other Ways That I Can Have A Baby?
Adopting a baby is also an option for people with HIV who want to begin, or expand their families. You can certainly enjoy parenthood with adoption as this means that you would have full legal responsibility for that child. You would also be giving a child a home.
If you would like to learn more, feel free to reach out to the Children’s Authority of Trinidad and Tobago.
Can A Couple Conceive A Baby Without The Uninfected Partner Becoming Infected?
Many couples in which one person is HIV positive and the other person isn't want to have children. With careful planning, it is possible to have a safe and successful pregnancy while preventing HIV from passing to the HIV-negative partner (or to the baby). It is very important to discuss your desires and intentions for childbearing with your health care provider before the woman decides to become pregnant. Your provider can help with decisions about how to conceive safely (if your provider is not familiar with reproductive issues for HIV, ask to see an HIV specialist).
Are There Any More Options For Fathering/Having A Child?
If you are a man living with HIV, the question above may be one that you have considered. While the typical means of conceiving may be some couples’ ‘go-to’ method, there are still other ways in which a person can begin or expand their/her/his family.
Although not currently available in Trinidad and Tobago, a discordant couple can access PrEP, in order to protect the HIV negative partner from getting the virus during sexual intercourse and conception. The negative person should start PrEP at their doctor’s recommendation and approval before the couple tries to have a child.
Another option for conception is through in vitro fertilization (IVF) and intrauterine insemination (IUI). Fortunately, in Trinidad and Tobago, we have two Fertility Treatment Centers that offer these services. They are the Trinidad and Tobago IVF and Fertility Centre and the Barbados Fertility Clinic.
For other questions on HIV and pregnancy,
call the National HIV Helpline 800-4HIV or 800-4448. (This is a toll-free number)
You are not alone. #youarenotalonett.
PREVIOUS TOPIC:
Comfort Care
NEXT TOPIC:
HIV and COVID-19
Events

UPCOMING
EVENTS
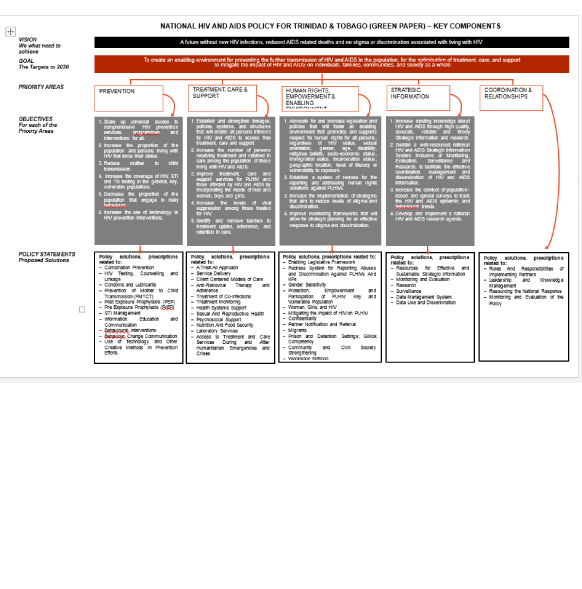
PUBLIC CONSULTATIONS ON THE NATIONAL POLICY ON HIV AND AIDS
Dear Stakeholders, The NACC wises to invite you to our upcoming consultations on the National Policy on HIV and AIDS. In persons consultations will be held on August 29th 2023 , September 7th and September 14th. Please indicate your preference for attendance by completing the registration link below.
Event Registrations for Public Consultations on The National Policy on HIV & AIDS
PAST & UPCOMING CALENDAR OF EVENTS & More
Training

TRAINING &
WORKSHOPS
COMING SOON!
PAST & UPCOMING TRAINING WORKSHOPS & More
Community Outreach

COMMUNITY
OUTREACH
COMING SOON!
SOCIAL RESPONSIBILITY COMMUNITY & More
Career

CAREER
OPPORTUNITIES
NO OPPORTUNITY PRESENTLY.
JOB OPENINGS, CAREER OPPORTUNITIES & More
Media

MEDIA
RELEASES
World AIDS Day 2022 -
December 1st
Unite to end the inequalities holding back the end of AIDS.
Since 1988, the world has celebrated World AIDS Day in remembrance of all those who have died of AIDS-related illnesses and those living positively and bravely with HIV. World AIDS Day remains as relevant today as it’s always been, reminding people and governments that HIV has not gone away. There is still a critical need for increased funding for the AIDS response, to increase awareness of the impact of HIV on people’s lives, to end stigma and discrimination and to improve the quality of life of people living with HIV. The human cost of inaction on AIDS is an injustice by governments and people alike, if action is not taken to end AIDS.